 The (PROWESS) study demonstrated that administration of recombinant human activated protein C (drotrecogin alfa) resulted in lower mortality (24.7%) in the treatment group versus placebo group (30.8%). With increased levels of APC present and its potential to decrease morbidity and mortality by pathways preventing progression to DIC, recombinant APC is being investigated in sepsis. Although one may argue that increased circulation of thrombin can lead to multi-organ microvascular thrombosis and death, thrombin is an essential activator of APC. We believe the mechanisms involved in FVL+/-, including resistance to cleavage by activated Protein C (APC), and increased thrombin formation help decrease mortality in patients with AFE, similar to what has been seen with sepsis in FVL+/- mouse studies. We explored whether alterations in the coagulation cascade, as seen in FVL+/-, can alter the progression to DIC. With AFE theorized to have mechanisms similar to the SIRS response of sepsis, we suspect factors that attenuate mortality in sepsis, such as DIC, may also have a similar result in AFE. Studies have shown that a FVL+/- carrier status in severe sepsis has been associated with improved survival in humans and mice. While criteria set by the Society for Maternal-Fetal Medicine (SMFM) and Amniotic Fluid Embolism Foundation for AFE diagnosis includes the development of DIC, DIC is not always present in the setting of sepsis or AFE. She was transferred to the postpartum unit on postoperative day 2 with an uneventful remainder of her hospitalization until discharge on postoperative day five.ĭiscussion: We present the above case as an atypical presentation of AFE. She was successfully extubated on postoperative day one following significant improvement in vitals, imaging, and was started on prophylactic Lovenox. While prognosis was initially guarded, the patient's condition drastically improved overnight. Shortly after the cardiopulmonary arrest, there was a high concern for AFE based on the clinical scenario and imaging findings. Additional lab findings showed 170 a fibrinogen level of 399 mg/dL and a normal coagulation panel and platelet range. No evidence of venous thrombosis was noted. Chest X-ray showed severe airway disease, and chest CTA further demonstrated airspace opacities in both lungs. She was transferred to the ICU, where she was started on Levophed for refractory hypotension. Return of spontaneous circulation was achieved following CPR and administration of a single dose of epinephrine. She lost palpable pulses, and CPR was initiated as intubation was performed. Approximately 30 minutes following surgery, the patient developed sudden onset of shortness of breath, tachypnea, confusion, cyanosis, hypotension, brady-cardia, and hypoxemia with an oxygen saturation of 21% despite supplemental oxygen. Emergency cesarean section was required due to an umbilical cord prolapse. Her pregnancy was otherwise uncomplicated. 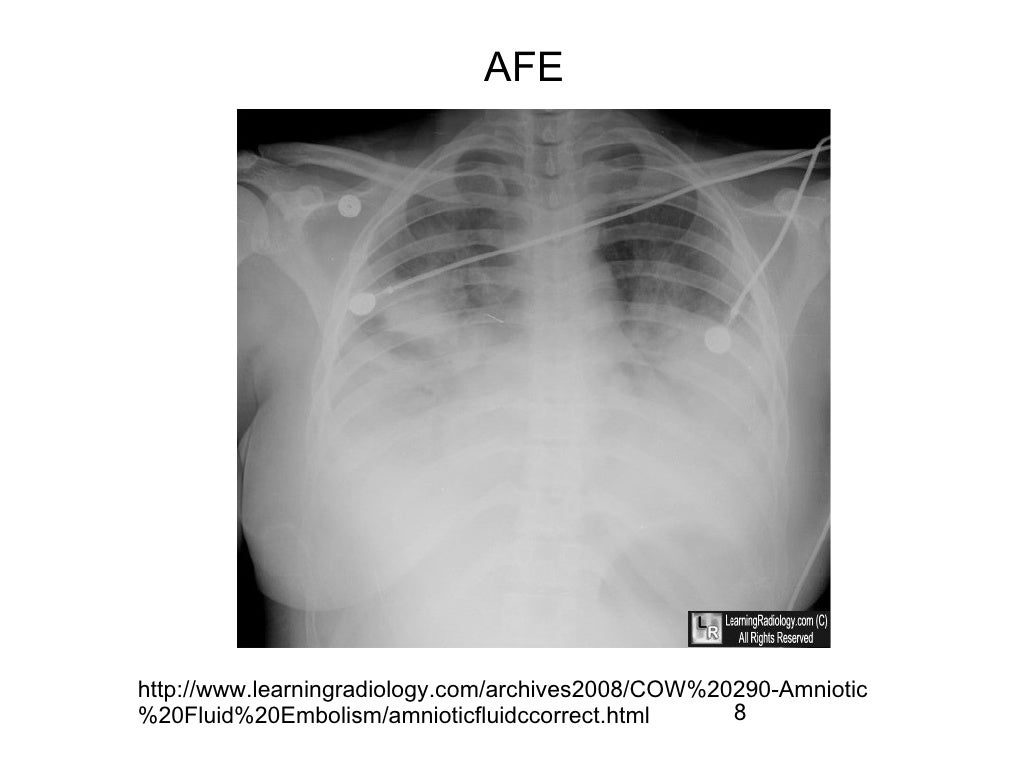
The following case describes the labor course of a patient with FVL+/- complicated by a postpartum AFE that did not progress to DIC.Ĭase Report: Patient is a 31-year-old G2P0 with a history of FVL+/- who presented for a scheduled induction of labor at 40 weeks and 5 days gestational age.  
Specifically, we ask if alterations in the coagulation cascade of heterozygous Factor V Leiden mutation (FVL+/-) can decrease mortality as seen in studies with severe sepsis. With similar theorized mechanisms, we suspect factors that may modify mortality in sepsis may also modify mortality in AFE. This often results in acute respiratory distress syndrome (ARDS), cardiopulmonary arrest, disseminated intravascular coagulation (DIC), and death. Background: Amniotic fluid embolism (AFE) is a rare and commonly fatal obstetric emergency theorized to trigger an inflammatory reaction much like the systemic inflammatory response syndrome (SIRS) of sepsis, leading to vascular constriction and coagulation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
